
On August 12, 2019 The Irish Independent published an article titled ‘When it comes to body fat: is it all about location, location, location?’ In the article, the author Katy McGuinness spoke with two professionals in the health care sector about menopause, the location of excess body fat and ways and means to reduce it.
Motivation Weight Management and Dr. Maurice Larocque, a physician and an expert clinical researcher in weight management, want to draw attention to a number of shortcomings in the article, specifically in relation to the general lack of understanding amongst healthcare professionals of the critical role that thoughts, willpower and motivation play in weight loss.
We have known for over 40 years that fat location around the waist is correlated with more medical illnesses such as type 2 diabetes, cardio-vascular disease and even cancer.
The Iowa study, which serves as the statistical basis for the article, shows that there is a 31% higher risk of dying when the waist is over 35 inches. This is what we call a Relative Risk (RR).
But what is important is the Absolute Risk (AR). We do not have the exact data here but with the 157,000 post-menopausal women examined, the AR is probably a lot under 1% and closer to 0,001%. Such small numbers are not really reliable.
The endocrinologist quoted in the article and his explanations about obesity, its causes and its treatments are highly revealing of the incomplete and confused medical view of the problem.
“If weight is going down, the internal interpretation is that we are in ‘famine mode’, so the body increases hunger to try to get us to eat whatever we can, and also simultaneously reduces our calorie burn.”
What I experienced in my 40 years expertise with over 20,000 patients is the opposite. After 3 days of following a VLCD (very low-calorie diet), the body will produce natural ketone bodies that curb appetite.
The endocrinologist adds, “Women should seek GP advice regarding medical and surgical options if diet and exercise intervention doesn’t work.”
In January 2019 in Cell Metabolism, a group of McGill University researchers in Montreal published this unique study: Neurocognitive and Hormonal Correlates of Voluntary Weight Loss in Humans.
I was part of this Dagher & al. study. We tested the hypothesis that hormonal adaptations during dieting override eating self-control in 24 overweight participants on a 1,200 kcal/day diet. We found that brain activity in cognitive control regions, rather than hormones associated with energy balance, plays a critical role in weight loss.
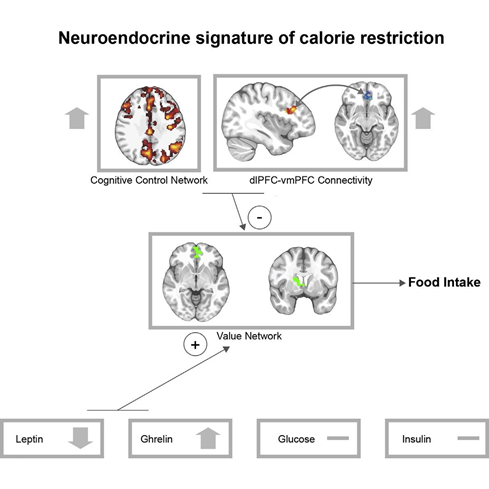 Study Highlights
Study Highlights
- We performed functional MRI in individuals who undertook a weight-loss regimen
- Calorie restriction led to weight loss and leptin and ghrelin adaptations
- We uncovered a neural signature of successful weight loss
- The best predictor of success was activation in prefrontal cortex during the regime.
This means that thoughts, willpower and motivation are the essential elements for success – not medication or surgery.
I deeply deplore the fact that medicine does not seem to see humans as a whole, comprising mind, body and spirit.
At this moment, there is no efficient medication, or surgery that cures the behaviour of people suffering from being overweight or obese.
We need to support and help the human being and stop treating obesity, ‘the disease’.
That is my call to doctors and there is hope.
Maurice Larocque md
Note: We’ve published a series of articles and helpful papers on menopause:



